Helps Patients, Providers, Payers and Communities

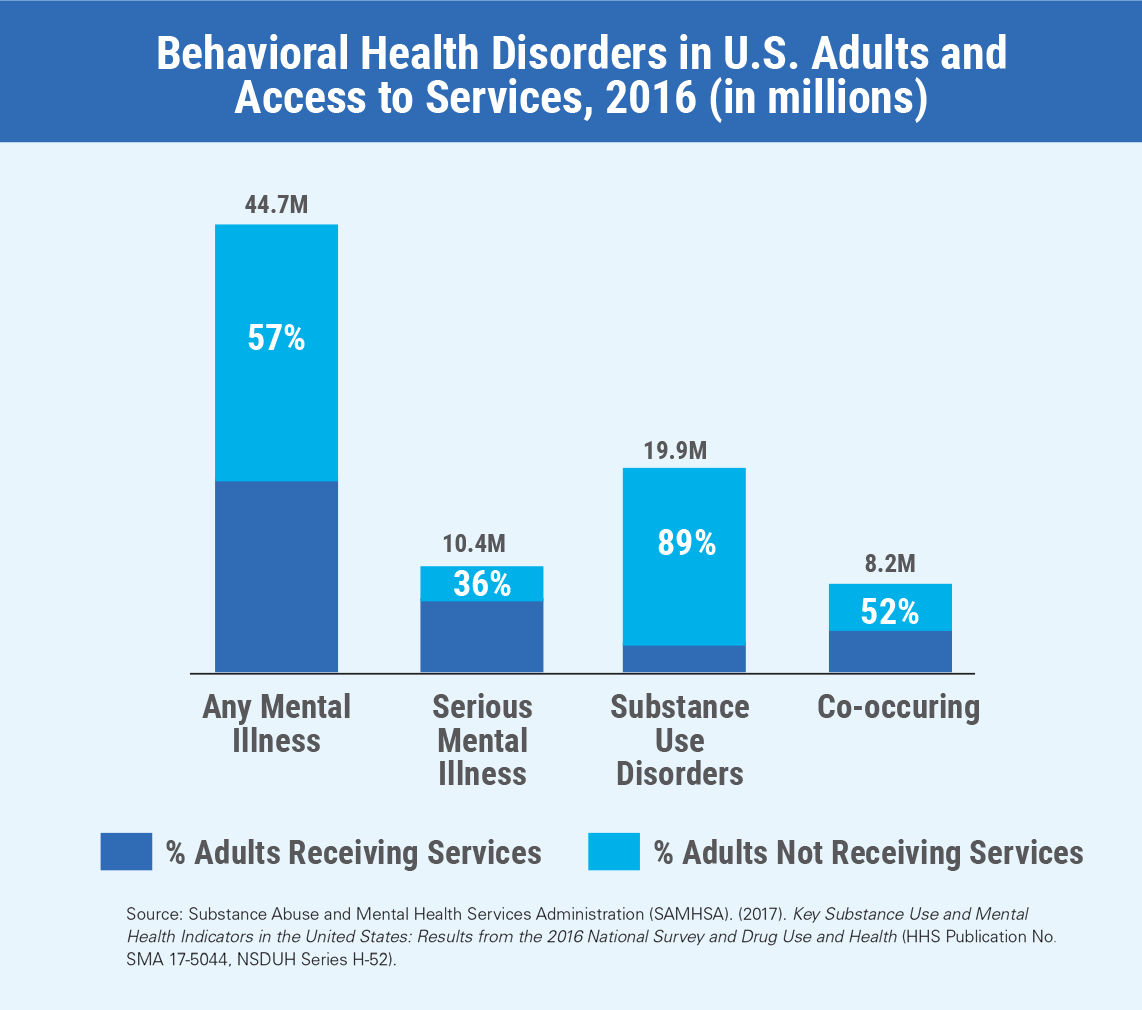
It should be no surprise to anyone that America’s healthcare system is experiencing a significant and increasing, need for high-quality behavioral health services. Research suggests that roughly 20% of the U.S. population may have behavioral health disorders, yet nearly 60% have unmet needs, which has a strong community-wide impact. This demand – particularly the nation’s rapidly-growing aging population – is not being adequately met.
This guide outlines how successful integration of behavioral health can meaningfully reduce medical expenditures and improve care delivery, and how partnership can create new efficiencies in management and administrative functions.
Unmet Behavioral Health Needs
Behavioral health includes mental illness as well as substance abuse disorders. Individuals requiring behavioral health solutions may suffer from either – or both – conditions. According to the American Hospital Association, “unmet behavioral health care needs among adults have increased demands on hospitals and health systems across the continuum of care.”
 Medical costs for treating patients with chronic medical issues along with behavioral health conditions are two to three times higher than for patients who don’t have comorbid mental health or substance abuse disorders. These comorbidities complicate care and negatively impact outcomes which further compounds costs to the system.
Medical costs for treating patients with chronic medical issues along with behavioral health conditions are two to three times higher than for patients who don’t have comorbid mental health or substance abuse disorders. These comorbidities complicate care and negatively impact outcomes which further compounds costs to the system.
Additionally, the COVID pandemic is putting new strains on individuals with mental health needs and has led to increased drug and alcohol abuse. Similar to the global financial crisis of 2007, it is expected that the nation will see higher rates of depression, anxiety and alcohol and drug use. The fear of the virus itself, prolonged social isolation, unemployment and collective grief compound the impact that the virus will have on behavioral health.
All of these complicating factors have led payers to seek new ways to improve overall health – behavioral and physical – of members or beneficiaries to reduce expenditures.
A Strategy to Reduce Total Health Expenditures
The optimization of an existing behavioral health unit and/or addition of a new BH service line has the potential to significantly cut costs. According to a recent Milliman Report, effective integration of behavioral healthcare with medical care can create projected annual savings of 9% to 17% when considering Medicare, commercial insurance and Medicaid enrollees.
Benefits of Partnerships in Care Delivery
In order to appropriately meet the current – and future – behavioral health needs of their patient populations, hospitals and health systems need a quality partner that can not only expand patient access but also effectively and efficiently manage a behavioral health program.
Joint venture relationships or contract management of behavioral health operations can address many of the challenges within the healthcare system by creating the best of all worlds. A recent study confirmed the benefits of joint ventures and partnerships, including “helping businesses grow faster, increasing productivity, and generating greater profits, both parties sharing the risks and costs, accessing new markets and distribution networks.” Some other common advantages of strong partnerships:
Quality Outcomes: Strong partners with a reputation for, and demonstrated success in, clinical excellence will drive high-quality outcomes for behavioral health patient populations and may help hospitals optimize value-based purchasing program performance.
Expanded or Stronger Service Offerings: A partnership can not only strengthen and expand existing services but also provide new offerings, such as inpatient behavioral health services, that are not currently available. This increased access enables more patients to receive treatment in an optimal care setting while reducing stress on ED departments.
Operational Efficiency: By having a partner fully dedicated to the behavioral health service line, the administrative burden is relieved and greater efficiencies are created.
Solutions
 Lifepoint Behavioral Health helps expand access to behavioral health services in local communities nationwide. We partner with hospitals and health systems to leverage expert medical, mental health, substance abuse and operational skills to improve clinical and behavioral health outcomes while lowering long-term patient costs.
Lifepoint Behavioral Health helps expand access to behavioral health services in local communities nationwide. We partner with hospitals and health systems to leverage expert medical, mental health, substance abuse and operational skills to improve clinical and behavioral health outcomes while lowering long-term patient costs.
As a division of Lifepoint Healthcare, our behavioral health program capitalizes on the company’s core competency as a partner who can effectively manage specialty programs for unique patient populations. We effectively leverage this operational integrity and established infrastructure to enable rapid expansion of behavioral health services.
Lifepoint Behavioral Health specializes in compassionate behavioral health services, including crisis stabilization for acute mental health and substance use disorders; detoxification from alcohol, opiates, cocaine and other drugs; suicidal thoughts or actions, anxiety, depression and post-traumatic stress disorder; and many other behavioral health illnesses.
Get in touch
Contact us today to learn how partnership with Lifepoint could benefit your hospital and community.

